We want to ensure that when we help our clients select the best Medicare Prescription Drug Plan (PDP) for their specific prescription  needs. As the annual enrollment period begins our clients are provide through the U.S. Mail a large number of advertisements to select the particular carrier’s prescription drug plans. They have great advertising literature that say some great claims of saving 80% on your prescriptions.
needs. As the annual enrollment period begins our clients are provide through the U.S. Mail a large number of advertisements to select the particular carrier’s prescription drug plans. They have great advertising literature that say some great claims of saving 80% on your prescriptions.
I can see how this can be very overwhelming as a person looking to help save on their prescriptions. The truth is the claims may be true for certain prescriptions, but how will the carriers plan do with your set of prescriptions? You cannot believe the information provided without doing additional research on what your prescriptions will cost. In some cases, you may find that that prescription plan advertisement you got in the mail may be 80% more expensive than another plan.
There is a tool out there I use as an agent to remove emotion and help select the best prescription plan for my clients. This tool is provided on Medicare.gov. I never though the tool from the government can be so useful to objectively look at the coverage from all the various options available in your area. The tool will let you select your prescriptions, your pharmacy, and show you your prescription costs monthly throughout the year. The site will show you when you fall into the Coverage Gap and estimate when you will reach the catastrophic coverage. The tool can give you piece of mind that you are actually going to find the best plan for your particular set of medicines.
To check you set of prescriptions is very easy to do with the help of your insurance broker, but you can do this by yourself. The Medicare.gov system will be able to save your prescriptions and zip code to allow you to visit again. This is great especially if you have many prescriptions. Once you are on Medicare.gov, you can select “Find Health and Drug Plans”.
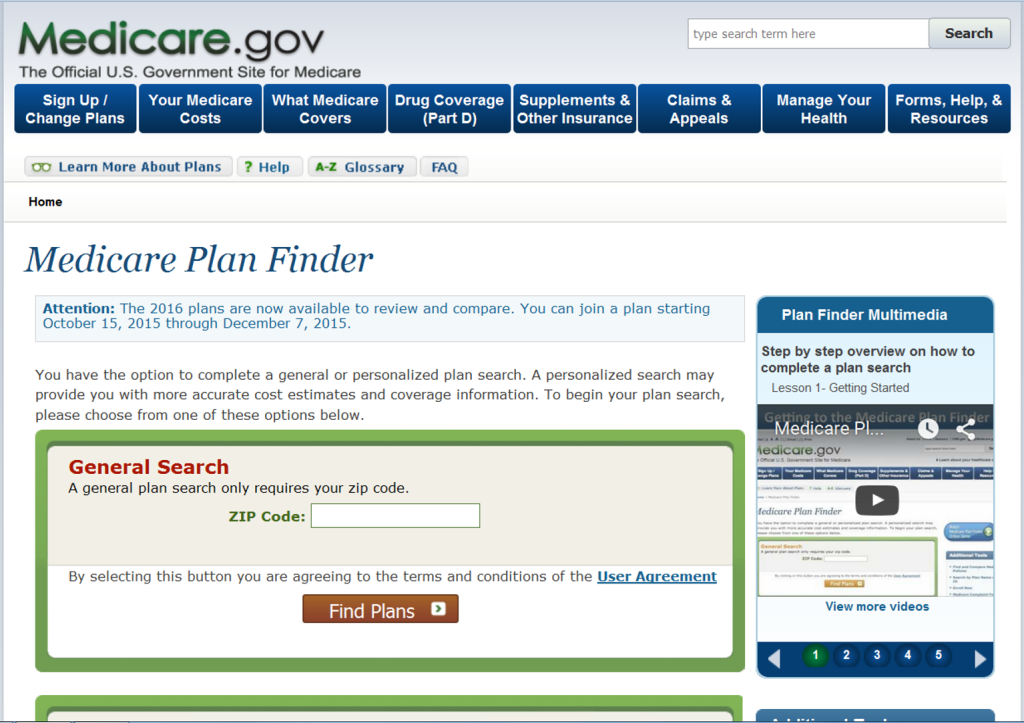
Once the new page opens you will enter your zip code.
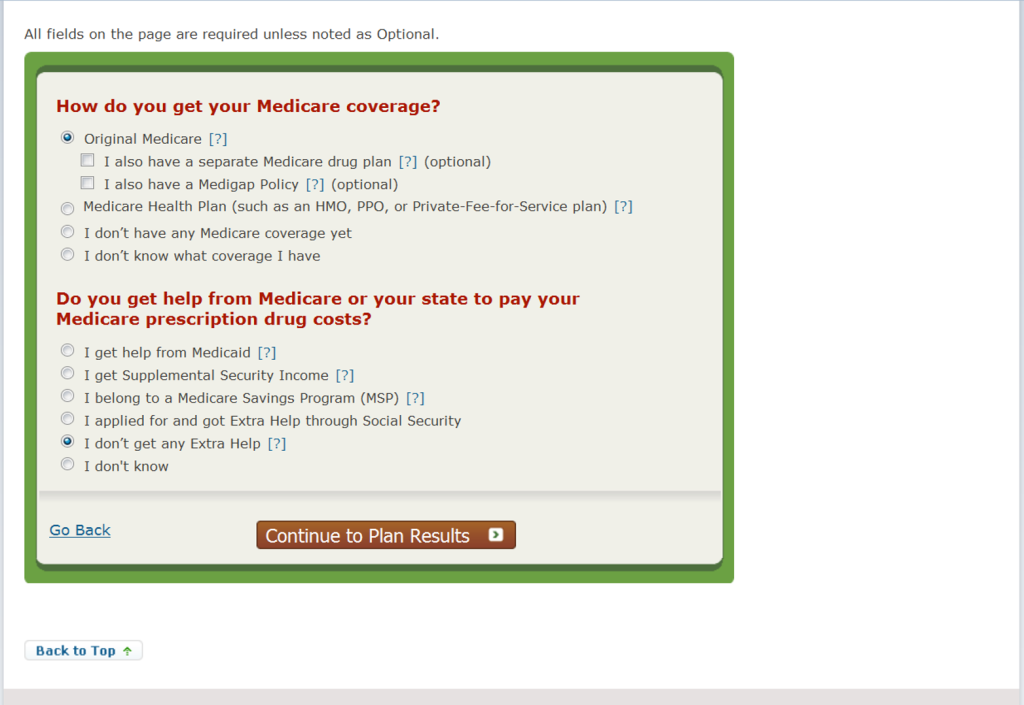
Next you will answer the questions “How do you get your Medicare coverage?“And “Do you get help from Medicare or your state to pay your Medicare prescription drug costs?” then click the “Continue to Plan Results”.
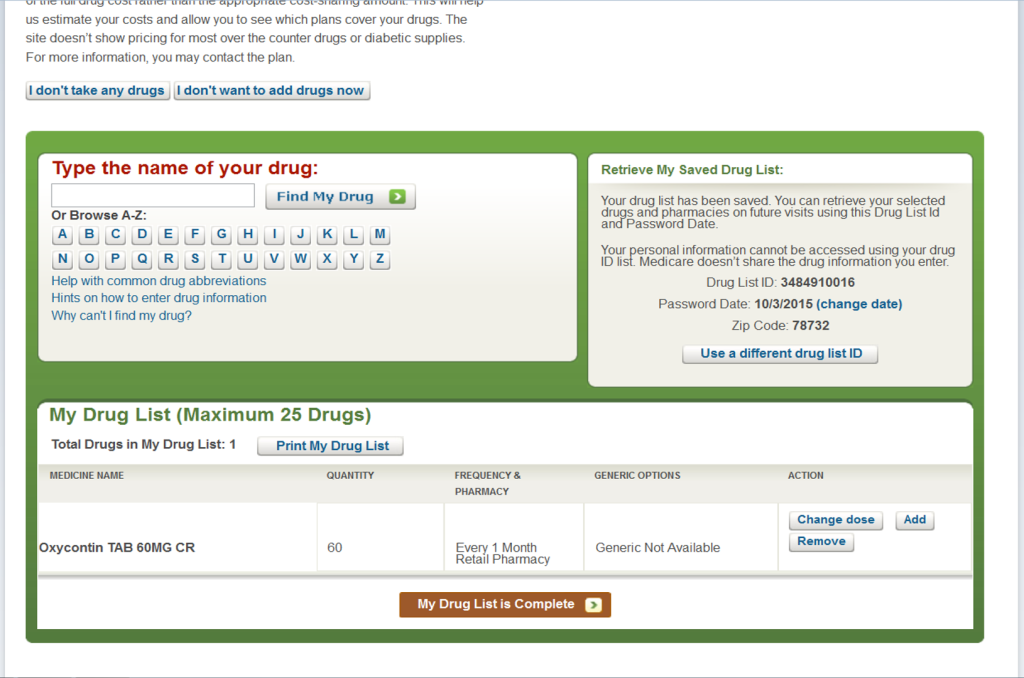
The next step is to enter your prescription drugs. Be very specific on your prescriptions, dosage and number of times a day that you take them. They will even ask how often you refill your prescription (monthly, 90-day or other).
Once you enter your first prescription, you will be able to save a couple of numbers that will allow you to retrieve your drug list.
Drug List ID: 3484910016
Password Date: 10/3/2015 (change date)
Zip Code: 78732
As shown below in the screen shot from Medicare.gov. If you have these 3 numbers you can return to the list at a later date.
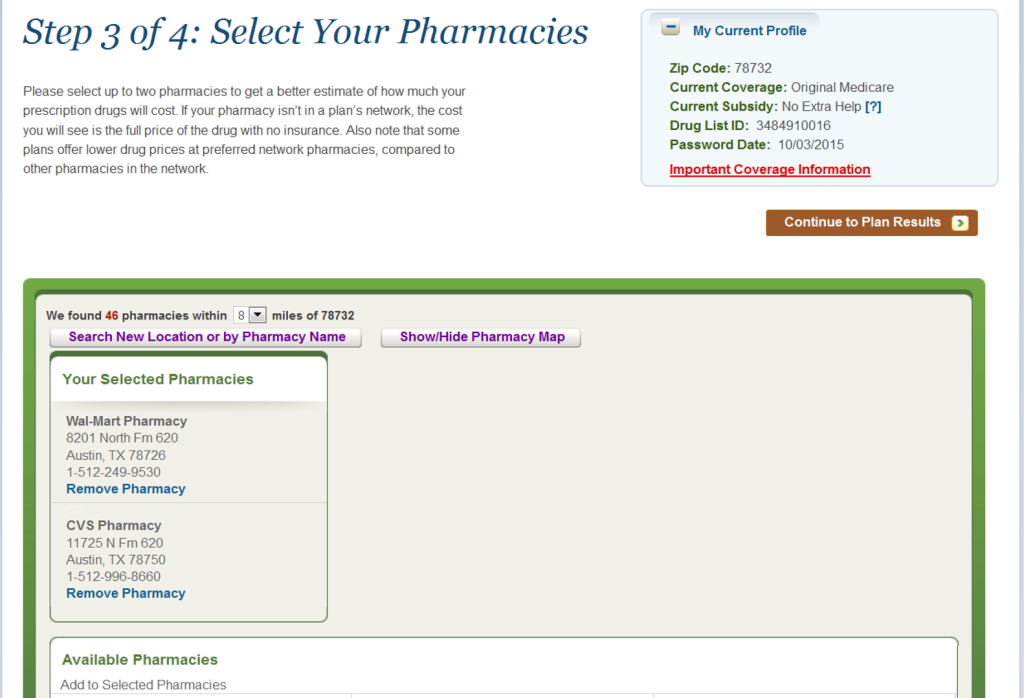
Once your drug list is complete, click “My Drug List is Complete”. You will then be able to select up to two pharmacies, your favorite one and one additional pharmacy.
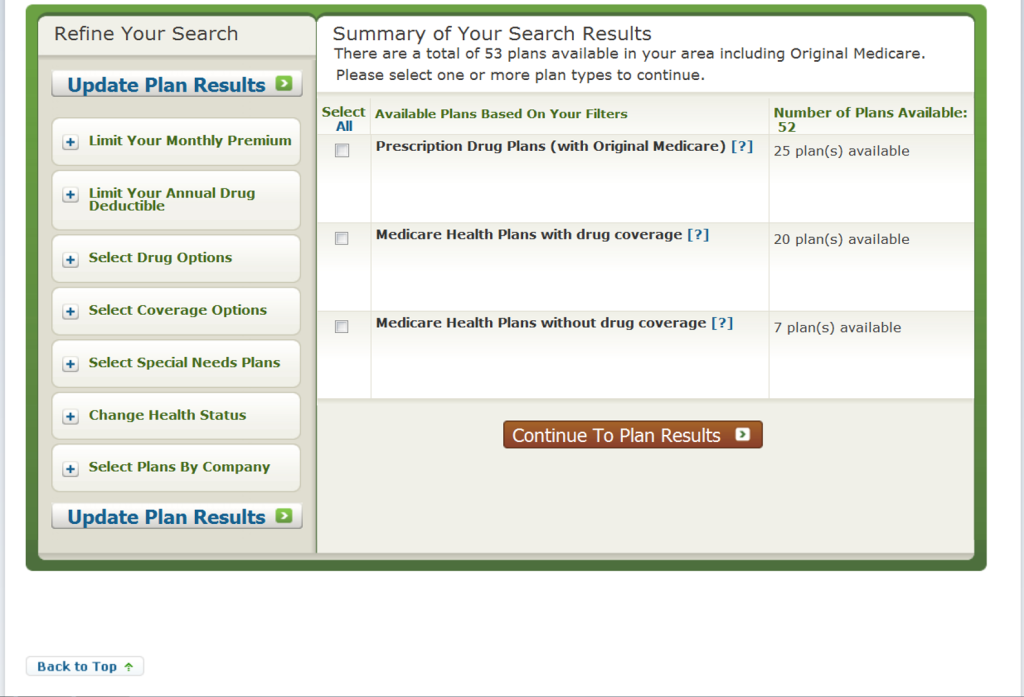
When you are done here, you select “Continue to Plan Results” Then you will be able to select if you want to look at Medicare Health Plans with Prescription drug coverage (MAPD) or Prescription Drug Plans (with Original Medicare) – the top two options.
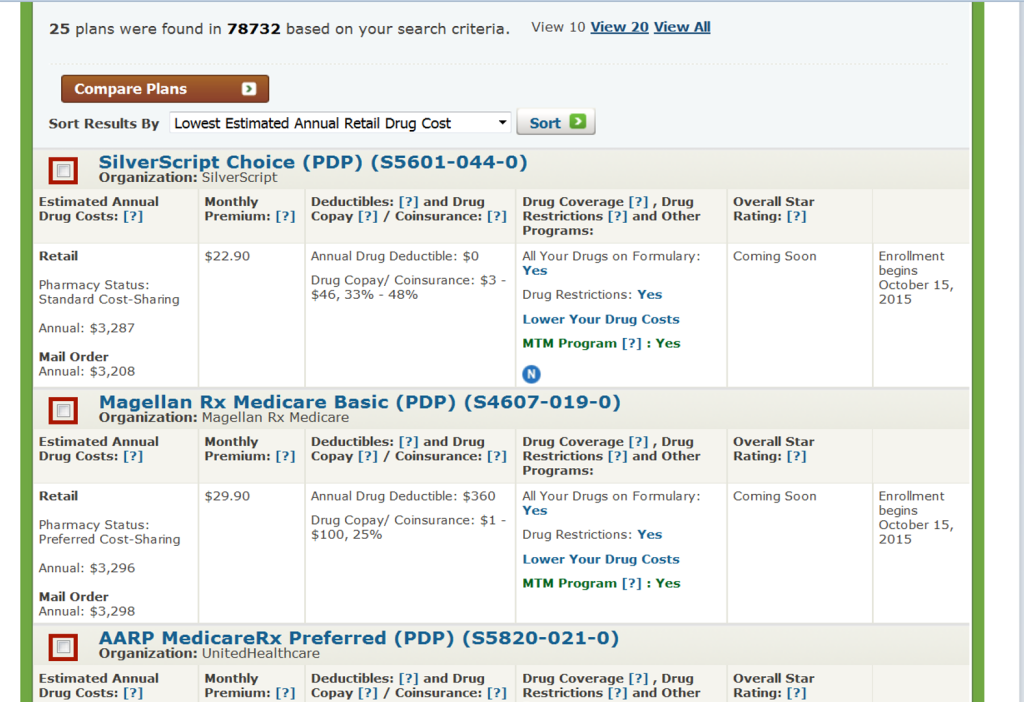
Next for this example I selected the Prescription Drug Plans. Original Medicare costs are always shown at the top of the list, but if you scroll down you will see the plans sorted by annual cost. The annual cost is the cost of your prescriptions at your first pharmacy and this includes the annual premium as well.
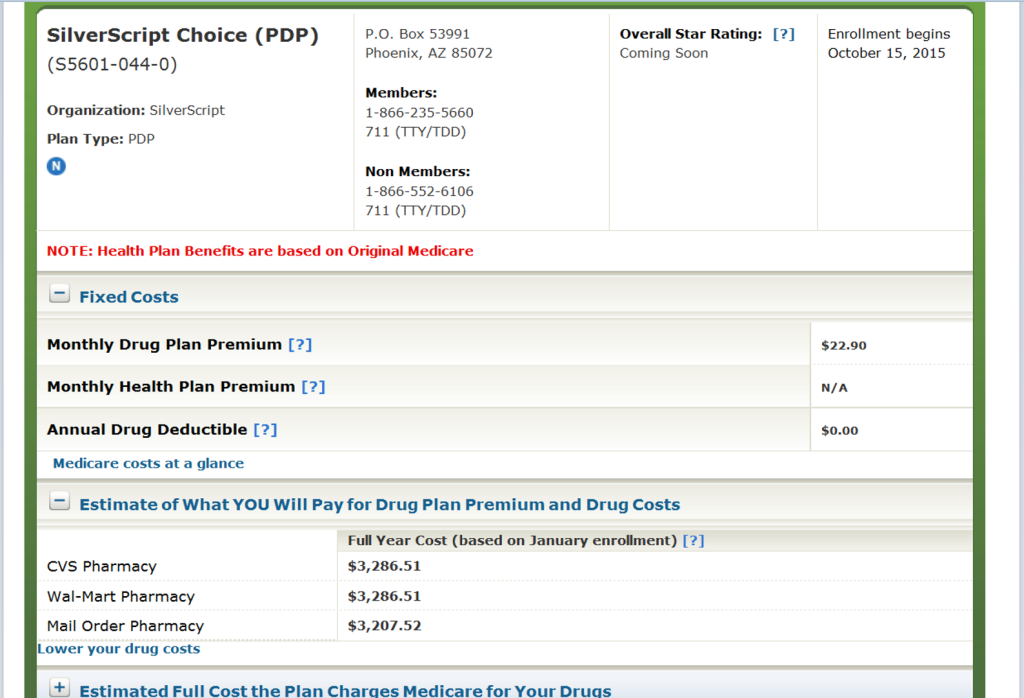
We can drill down even more on the plan by clicking the “SilveScript Choice (PDP) title and see further details on your cost.
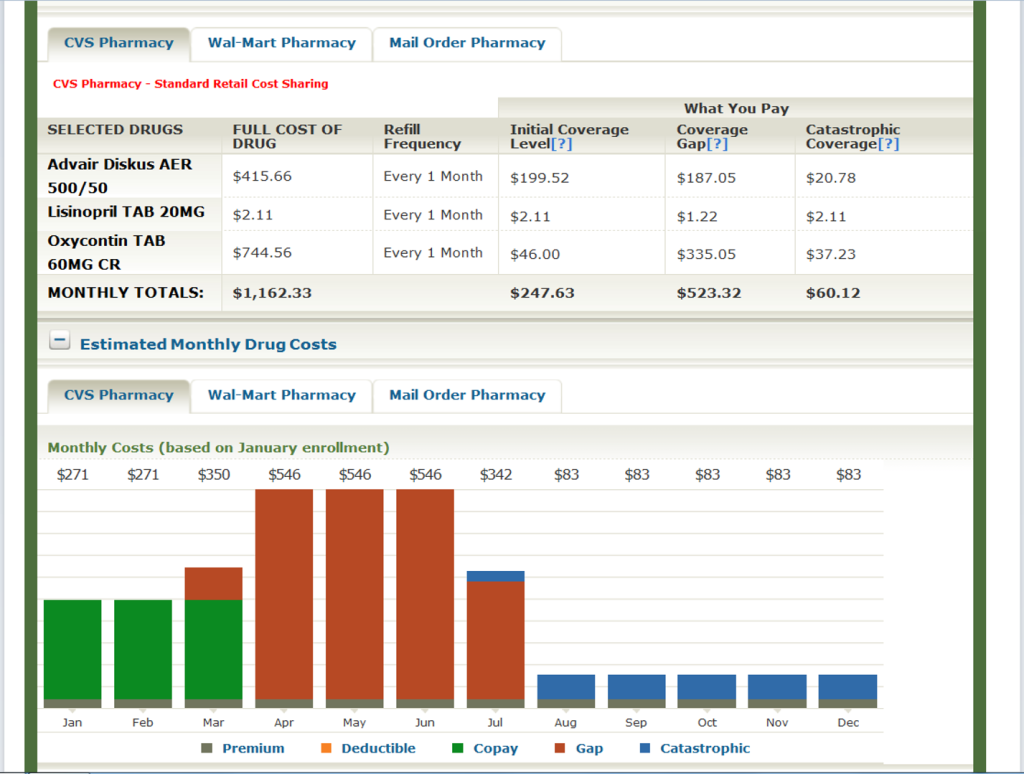
Two things are very clear on this top part of the details – the plans Star Ratings, how well the plan is rated by a variety of factors, the plan monthly premium, and the annual drug deductible. As you move further down the page, you can see the annual costs for premium and drugs at each pharmacy option and through the mail order program included with the prescription drug plan.
In the above chart there is a lot of information to help you review the costs for this plan on your prescription drugs. They show you the Full Cost of the Drugs, this is the retail cost for each drug on the plan. The Initial Coverage Level, this is the cost for the prescriptions you would expect to pay at the pharmacy for each prescription (shown in Green on the bar graph). The cost you will expect in the Coverage Gap (Donut Hole), shown in brown in the bar graph. The cost of your drugs in the Catastrophic Coverage, shown in Blue on the bar graph. The monthly premium is shown in grey on the bar graph. This graph can help you plan when you hit the Coverage Gap.
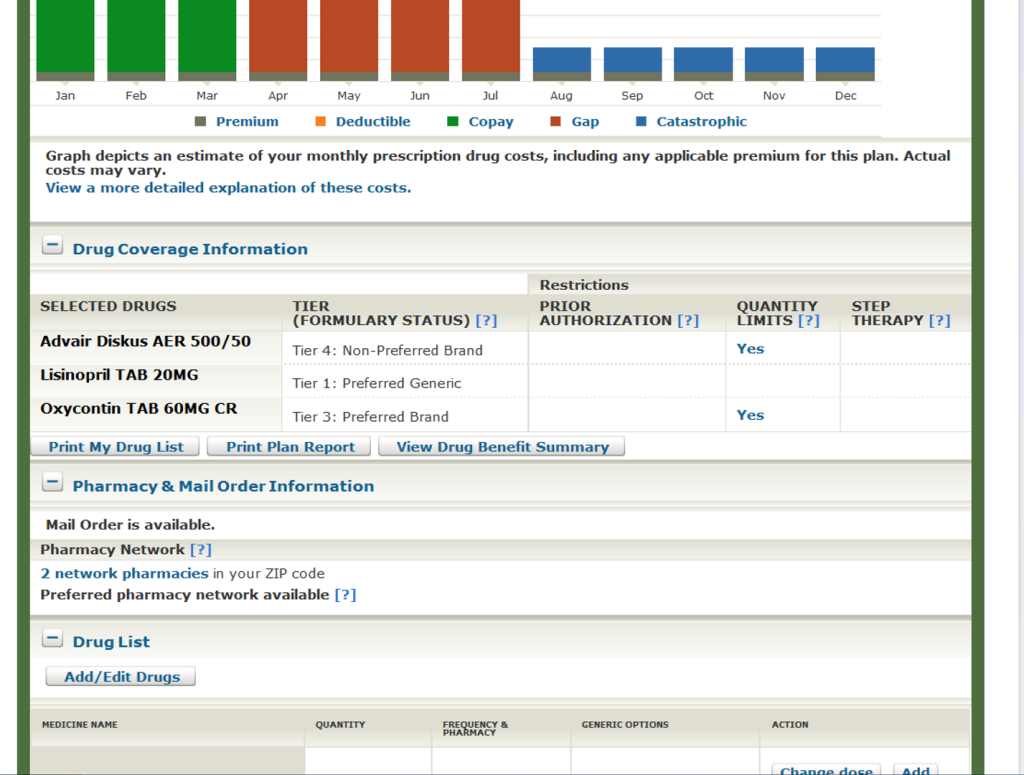
As you get close to the bottom of the plan details, they tell you what tier each medication is on the plans Formulary. They will as well tell you if your prescription is not covered on the Formulary.
When I help my clients we walk them through this level of detail to do the best job we can at estimating costs for them. We have found this Medicare.gov site is a great resource that can be very objective with the clients specific set of medicines. This is a free tool and gives you the most comprehensive estimate of your RX costs and plan costs throughout the year.
If you do have questions visit with a local broker to help you through the process. There is no extra cost for having someone help you find the best options. Don’t miss your change to make a change of plans if there may be a better option out there for you. The Annual Enrollment Period is October 15th through December 7th each year. Plan evaluation is an important part of your annual review of your coverage.